Disclaimer: The information on this site is for educational purposes only and is not a substitute for professional medical advice. Only a licensed medical professional can diagnose any illness. Please talk to your doctor before stopping or starting any treatments or making changes in your diet or exercise.

Food and diet are among the hottest topics of discussion (and the most controversial) when it comes to living with CKD. There is so much outdated, false information on the internet, and a lot of the things you hear on social media are unrealistic and based in fear-mongering. Especially when you have a second condition like diabetes or high cholesterol, adhering to the traditional “kidney diet” can seem contradictory and it may even feel impossible. So what are we supposed to do when it feels like everything is off-limits? Here are some tips to help you navigate your dietary needs.
Start by speaking with a renal dietitian. This is probably the most impactful thing you can do for your kidney health outside of listening to your nephrologist and taking your medicine. A renal dietitian is highly trained and knowledgeable, and has received additional certifications to be able to work specifically with kidney patients and their individual needs. Since your kidney diet will be influenced by many different factors, a renal dietitian can help you learn what foods will work best for you. When I saw my renal dietitian for the first time, she provided me with several lists of produce, packaged snacks, protein, beverages, and other food items that would fit in with my nutritional requirements. She taught me how to use those lists to create balanced and healthy meals that I would actually prepare and eat. A renal dietitian will base their recommendations on your personal lab results, as well as your preferences and any sensitivities or allergies. They can also help you choose items that will work with other dietary needs, like lower-carb foods for diabetic patients and high fiber for controlling cholesterol. Working with a professional will take all of the guesswork out of your dietary planning.
Learn what you need to avoid—and why. It’s not really enough to simply know that your dietitian or nephrologist has asked you to cut back on a certain food or drink, you should also know why that recommendation was made. For example, many of us are told to avoid drinking dark-colored sodas, but some of us aren’t aware that dark soda itself is not the enemy, it’s the phosphorous that’s causing issues. There are dark sodas that don’t contain any phosphorous and could be totally safe to drink, but on the other hand there is hidden phosphorous in plenty of other foods, like processed meats. There are so many other examples like this one, probably too many to list. These little tidbits of information are important, since you need to be aware of exactly what it is you’re looking out for. It’s your responsibility to be informed about this so you can stay in control.
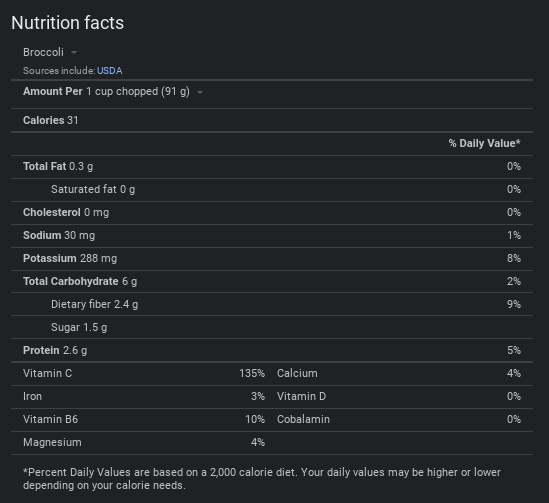
Get comfortable with reading nutrition labels. The label on the back of the container should be the first thing you check when you find yourself asking, “Is this safe for me to eat?” Nutrition facts are listed on the back of most packaged food, by law. The information listed will give you a clear picture of what type of nutrients you will find in a serving of that item. Work with your dietitian or nephrologist to learn what a reasonable amount of sodium, potassium, protein, etc., is for you per serving or meal. You can even check the nutrition facts for produce online! A web search will show you the “label” for a serving size of any vegetable or fruit you can think of.
Understand that it’s not one-size-fits-all. Some patients need to limit sodium, potassium, protein, phosphorus, oxalates, or a combination of all of the above. Meanwhile, other patients may have very minimal restrictions—or none at all. Take a look at your most recent lab results and see which numbers are out of range. If something is high in your labs, that means cut back on it in your diet. If your potassium levels are normal, then you probably don’t have to stop eating spinach or tomatoes. Our bodies actually depend on these nutrients, so if you’re severely cutting back on sodium or potassium while your blood levels are normal, you could end up with a deficiency. The recommended diet for someone in Stage 2 looks very different than the diet for a patient on dialysis. If you’re not sure whether you should be cutting back on something or not, ask your nephrologist or dietitian before making changes.
There a lot of myths out there, question everything. Don’t be afraid to do your own research if something sounds weird. A lot of people still think that Himalayan salt is “better” for the kidneys than table salt, or that kidney patients should always double-boil potatoes, or that white rice and white bread are better options than brown rice or whole grain bread. Unfortunately, there is a lot of misinformation online, and we have to be prepared to recognize it and sift through it.
Social media is great, until it’s not. Facebook, Pinterest, Instagram, and TikTok are wonderful places to find kidney-friendly recipes. You’re sure to find something that will work for you, even if you have to tweak the recipe or substitute a couple of ingredients. The downside to using social media as a guide is that this is where the majority of misinformation and fear-mongering can be found. Some of the advice given by individuals online, even if well-intentioned, can be terribly wrong or even downright dangerous. I’ve seen people on social media suggest juice cleanses and “carnivore” diets, both of which can cause serious problems for patients with CKD. It’s important to double check with your nephrologist or renal dietitian before you make any dietary changes, especially if you learned about it from a peer and not a professional.
Everything in moderation. It took me a while to understand that “moderation” applies to restricting, too. Our kidneys don’t know what a “cheat day” is, and they don’t get to take a break from their work. However, we have to eat in a way that’s sustainable for our lifestyle and mental health. There are celebrations, group dinners, holidays, travel, and other times where it might not be feasible to follow our recommended diet perfectly. It’s okay to have time off from your strict diet, as long as you keep your meals reasonable. For example, if you normally limit potassium, it should be okay to have a few banana slices in a fruit salad at a family gathering, but it would not be a great idea to eat 2 bananas each day for a week just because you’re on vacation and it’s the quickest thing to grab. Similarly, if you suffer from fatigue and you can’t reasonably keep up with preparing 3 healthy meals a day from scratch, it’s okay to ask for help or look for alternatives, like meal-prep services.
When in doubt, opt for lean protein, vegetables, and whole grains. If you’re still confused and you aren’t able to see a professional right away, the best thing you can do is choose traditional healthy foods. Especially if you’re in an early stage of CKD, or maybe not even diagnosed yet, you do not need to be taking extreme measures. Wait until a medical professional reviews your lab work and makes recommendations for you. You can do more harm than good by unnecessarily restricting your diet, so it’s best to eat well-balanced nutritious meals until you are told specifically what changes to make. Some good options include leafy greens, whole grain breads and pasta, lean chicken or fish, and an assortment of fruits and vegetables.
